Alcohol and the thyroid may be a toxic combination depending on the individual. Some research says alcohol in moderation can be beneficial but this does not always take into account individual health concerns.
This post explores the relationship between alcohol, the liver, and the thyroid. It discusses the effects of alcohol consumption on organs in the digestive tract and alcohol recommendations for those with suspected thyroid disorders.

Some of these links are affiliate links, which means when you sign up or purchase from these links we may receive a small commission at no extra cost to you. However, we only promote products and services that have provided insight and been very helpful to us. Thyroid Nutrition Educators is also a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Learn more about our disclosure statement here.
Relationship Between Thyroid & Liver
The thyroid is a butterfly-shaped gland that sits low on the front of the neck below Adam’s apple. This endocrine gland secretes triiodothyronine (T3) and thyroxine (T4). These hormones control various metabolic processes including basal metabolic rate (BMR) for all body cells including hepatocytes in the liver.
Role of the Liver In Thyroid Hormone Metabolism
The thyroid and liver have a symbiotic relationship. As a result, the liver needs T3 and T4 for optimal function and the thyroid needs the liver to metabolize and distribute its hormones.
The hypothalamus and pituitary gland in the brain control the thyroid through the hypothalamic-pituitary axis.
If thyroid hormone levels get too low, neurons in the hypothalamus release Thyroid Releasing Hormone (TRH) telling the pituitary gland to secrete thyroid-stimulating hormone (TSH). TSH tells thyroid cells to release T3 and T4.
The thyroid hormone mainly secretes T4 with som T3. T4 consists of about 80% of thyroid hormones.
There are 2 forms of T4: free T4 and plasma T4. Plasma T4 is bound to proteins and unable to enter body cells.
Liver Metabolizes & Transports thyroid hormones
The liver metabolizes and transports thyroid hormones.
The liver extracts more thyroid hormone than the thyroid delivers. About 5 to 10 percent of plasma T4.
T4 is converted to the active thyroid hormone T3. This consists of about one-third of the T4. Afer that it is sent to peripheral tissues to be synthesized into T3.
The liver is responsible for 30 to 40 percent of these conversions and provides a large pool of thyroid hormones available for the body to use.
Thyroid hormones also play a role in the liver’s ability to digest fat.
Thyroid dysfunction may impair liver function and liver problems will affect thyroid hormone metabolism. So ultimately, a problem in one of these glands can lead to issues with the other.

How Thyroid Conditions Affect the Liver
Thyroid conditions affect both the function and structure of the liver. This includes hypothyroidism, hyperthyroidism, and autoimmune conditions Hashimoto’s and Graves’ disease, as well as thyroid cancer.
HYPOthyroidism and the Liver
Hypothyroidism decreases the liver’s ability to excrete waste products. Reductions in wastes like bile and bilirubin can manifest into conditions including:
- Jaundice
- Gallstones
- Elevated cholesterol levels
- Nonalcoholic fatty liver disease (NAFLD)
HYPERthyroidism and the Liver
It is harder to pinpoint if the thyroid is the root cause of liver dysfunction in those with an overactive thyroid.
Hyperthyroidism may cause an insufficiency amount of blood and oxygen delivered to the liver. It can also lead to bone disorders. Changes in liver enzymes are one sign of dysfunction:
- Aspartate aminotransferase (AST) elevated
- Alanine aminotransferase (ALT) elevated
- Alkaline phosphatase (ALP) elevated
Chronic liver conditions including fatty liver and cirrhosis were a big risk of hyperthyroidism but new medical treatments have made these only rare occurrences today.
Some thyroid treatments may also elevate liver enzymes. The dose of medication can elevate levels. So it is important to monitor liver function.
Thyroid Autoimmune Diseases and the Liver
Thyroid autoimmune diseases may cause liver abnormalities and possibly result in the following liver conditions:
- Primary Biliary Cirrhosis (PBC)
- Chronic Autoimmune Hepatitis
- Primary Sclerosing Cholangitis
- Non Alcoholic Fatty Liver Disease (NAFLD)
Primary Biliary Cirrhosis (PBC)
Thyroid dysfunction occurred both before and after the diagnosis of PBC. Ten to 25% of PBC patients had autoimmune hypothyroidism. Antibodies were also present in this condition:
- 34% of PBC patients have Thyroid Peroxidase Antibody (TPO) antibodies
- 20% of PBC patients have thyroglobulin antibodies
Chronic Autoimmune Hepatitis
Thyroid conditions in chronic autoimmune hepatitis are also common.
Twelve percent of patients also had autoimmune hypothyroidism. Six percent of cases also had Graves’ disease.
Primary Sclerosing Cholangitis (PSC)
Primary Sclerosing Cholangitis (PSC) is a disease that affects the ducts that carry bile from the liver to the small intestine. It occurs when inflammation causes scars on these bile ducts. The following thyroid autoimmune conditions had an association with PSC:
- Hashimoto’s thyroiditis
- Graves’ disease
- Riedel’s thyroiditis, rare, chronic inflammatory thyroid disease
Non Alcoholic Fatty Liver Disease (NAFLD)
Non Alcoholic Fatty Liver Disease (NAFLD) can occur with both hypothyroidism and Hashimoto’s.
Inflammation from thyroid autoantibodies could also play a role in the development of NAFLD.
The thyroid is responsible for blood sugar and fat metabolism. A fatty liver can develop when the thyroid is compromised
Thyroid Cancer and the Liver
Though rare some patients have experienced secondary malignancies of the liver in differentiated thyroid cancer.
Seven out of 14 cancer patients had liver metastasis when first diagnosed.

Alcohol Is A Drug that Changes the Body
Alcohol is used for relaxation, stress relief, and also in social or celebratory events. The legality of this substance makes us forget that alcohol is a drug that has major physiological effects on all body systems including the thyroid.
When consumed alcohol alters mood, impairs cognition, and acts as a sedative. So it may lead to stimulation, depression, euphoria, sleepiness, heightened or reduced anxiety, and possibly physical addiction.
Research On Alcohol’s Physiological & Health Effects
Global statistics indicate that consuming alcohol is the third-highest factor in disease progression worldwide leading to about 260 conditions.
A review of the literature shows that there is no benefit from drinking alcohol. The study did not discriminate against wine, beer, or liquor but said overall most deaths come from any alcohol use.
There are also countless studies showing the benefits of certain alcoholic drinks in moderation. Most research is generalized and may not apply to every group of individuals.
In addition, it also shows the negative effects of alcohol consumption on the digestive system.
Alcohol Digestion Has Negative Effects on Health
Elimination of toxic compounds is part of metabolism. This is what happens during alcohol digestion. From the moment alcohol touches the mouth the body’s main goal is to eliminate it as fast as possible.
Alcohol Provides Energy But No Nutrition
Alcohol is not a nutrient. It only provides energy but no other health benefits.
Digestion of other nutrients leads to storage in organs and tissues. The only place you will find alcohol is within body water.
If alcohol accumulates in the blood it will destroy cells and tissues. To prevent this from happening the body oxidizes alcohol and removes it from the blood. A small amount is also excreted in the breath and urine.

Enzymes Facilitate Alcohol Digestion
There is a three-step process that occurs during alcohol digestion. Enzymes are compounds needed for alcohol metabolism. They help break down food and drink compounds. The enzymes responsible for alcohol digestion are alcohol dehydrogenase (ADH), aldehyde dehydrogenase (ALDH), and microsomal enzymes.
These enzymes break down alcohol and eliminate it from the body.
Alcohol Dehydrogenase (ADH)
Alcohol Dehydrogenase (ADH) is known for metabolizing vitamin A. This is the first enzyme that works to digest alcohol. Found mostly in the liver, ADH converts alcohol into acetaldehyde through a chemical process called oxidation.
Even in low concentrations, acetaldehyde is a highly toxic substance. This carcinogen is deadly to the body.
Aldehyde dehydrogenase (ALDH)
Aldehyde dehydrogenase (ALDH) is the next enzyme in alcohol digestion. This enzyme oxidizes acetaldehyde into acetate taking place primarily in the liver.
Acetate is a less toxic byproduct. It will leave the liver for use in the metabolism of other nutrients (carbs, fat, excess protein).
Acetate is then broken down into water and carbon dioxide for easy elimination.
Microsomal Enzymes Oxidizing System (MEOS)
The microsomal enzyme oxidizing system (MEOS) also metabolizes alcohol. This alternative alcohol metabolism uses microsomal enzymes called cytochromes.
These enzymes are responsible for only a small fraction of alcohol digestion. MEOS leads to a production of free radicals and may lead to cell damage.
Cytochromes in cells protect the body from harmful substances that enter the body.
MEOS oxidizes alcohol into acetaldehyde by the liver enzymes cytochromes P450, 2E1, or CYP2E1 and catalase.
Alcohol activates these enzymes. Increases in alcohol consumption lead to an increase in the number of CYP2E1 cytochromes. More alcohol will then become oxidized.

Effects of Alcohol on the Digestive System
Negative effects of alcohol on the digestive system occur due to the production of acetaldehyde and other free radicals given off during alcohol digestion.
The enzymatic activity of MEOS gives almost every cell the ability to metabolize alcohol leading to toxic byproducts across the whole body.
Alcohol consumption affects gastric motility depending on the percent concentration of the alcohol. Anything above about 15 percent tended to slow digestion.
Alcohol metabolism occurs throughout the digestive system. It affects the mouth, throat, esophagus, liver, pancreas, and anus.
Effects of alcohol on the digestive system include the following:
- Damage to digestive organs (mouth, throat, esophagus, stomach, liver, gallbladder, pancreas, intestines)
- Nutrient depletion and deficiencies
- Changes in hormone function
- Decreased immune function
Effect of Alcohol on the Mouth and Throat
Acetaldehyde is in tissues around the teeth and gums. This makes the mouth another source for a significant amount of alcohol metabolism.
This substance can damage the mouth and lead to cancer of the mouth and throat.
The more alcohol consumed the higher acetaldehyde levels become.
Just half a bottle of wine can lead to elevated levels of acetaldehyde and cause damage to DNA in oral cells of both humans and primates.
Alcohol changes the oral microbiome.
A study of 1,044 adult participants, aged 55–87 showed heavy and moderate drinkers had a higher amount of the harmful bacteria pathogens including Bacteroidales, Actinomyces, and Neisseria in their mouths when compared with nondrinkers.
Production of healthy bacteria like Lactobacillales decreased as alcohol consumption increased.
Certain bacteria such as Streptococcus and Neisseria bacteria produced acetaldehyde which increases the toxicity risk.
Effect of Alcohol on the Esophagus
The enzyme ALDH in esophagus tissue indicates alcohol metabolism takes place here. Chronic alcohol consumption can increase cell damage and the risk of esophageal cancers.
Effect of Alcohol on the Stomach
When exposed to alcohol there is damage to stomach cells. Acetaldehyde and other byproducts of alcohol digestion may also hinder the function of the stomach.
Alcohol can irritate and wear away the stomach lining leading to a gastric ulcer or perforation of the stomach wall. Peritonitis or inflamed stomach lining can also occur as a result of alcohol consumption.
Aside from physical damage, alcohol interferes with the production of stomach acid. It also obstructs muscles surrounding the stomach affecting gastric emptying.
Even when consumed with a meal alcohol decreases stomach emptying than when there is no alcohol intake.
Fermented beverages beer and wine emptied from the stomach much slower than whisky and ethanol.
Alcohol Digestion Enhanced by Carbohydrate Metabolism
Some individuals can also produce alcohol in their stomachs as a byproduct of carbohydrate metabolism. Levels can be as high as 0.35. Thi is about 4 times as high as the blood alcohol levels for intoxication. Alcohol production results from either of the following:
- Bacterial overgrowth from the breakdown of carbohydrates due to decreased stomach acid
- Food remains in the stomach for an extended period
The speed of gastric emptying also affects the activation of ADH and MEOS enzymes. Slow gastric emptying increases the production of acetaldehyde causing damage to the stomach.
Effect of Alcohol on the Pancreas
The pancreas exhibits ADH and ALDH enzyme activity. This means alcohol metabolism that takes place there. Enzyme activity was higher in men than women putting them at greater risk for health issues.
Alcohol and the production of acetaldehyde irritate cells of the pancreas and cause them to swell. Swelling leads to blockages of the pancreatic ducts and acinar (exit) cells that move enzymes out of the pancreas.
Byproducts from alcohol digestion also trigger the early activation of digestive enzymes within the exit cells. This causes the pancreas to digest itself resulting in cell damage, inflammation, and calcification. Over time this leads to fibrosis of the pancreas.
This pancreatitis often occurs in alcoholics, but some individuals may develop this condition with intake as low as 20 grams or 2 drinks a day. Excess consumption of 200 grams per day has also developed into pancreatitis. Some may never develop the condition no matter how long their drinking habits.
Other pancreatic complications include leakage of pancreatic fluids which can lead to jaundice, pseudocyst formation, malabsorption, and diabetes.
Effect of Alcohol on the Gallbladder
The effects of alcohol on the gallbladder are somewhat unknown. Alcohol consumption of 10 grams per day decreases the incidences of gallstones by 12 percent.
Alcohol consumption may also weaken the gallbladder and cause decreased gallbladder emptying. Those with gallstones also have decreased emptying.
Consumption of red wine, whisky, and 13.7% vol or 43.5% volume ethanol rapidly decreased gallbladder emptying times when compared with a solution of isotonic glucose.
Alcohol’s suppressing effect on the gallbladder may have to do with the concentration of alcohol within body tissues. It can also be a side effect of the slow gastric emptying that happens after alcohol consumption.
Fermented beverages beer and wine emptied much slower than whisky and ethanol on an empty stomach.
Effect of Alcohol on the Intestines
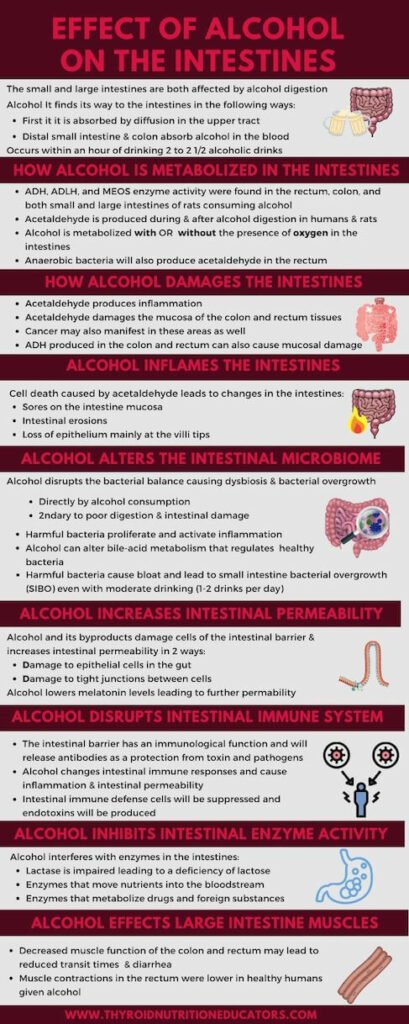
Alcohol digestion can affect both the small and large intestines. Alcohol finds its way to the intestines in a few ways.
When alcohol absorbed by diffusion in the upper tract when it is first consumed.
The distal small intestine and colon also absorb alcohol circulating in the blood. The concentration of these levels can reach up to 200 mg/100 mL within an hour of drinking 2 to 2 1/2 standard alcoholic drinks.
The Metabolization of Alcohol In the Intestines
Rats consuming an alcoholic diet for one month had ADH, ADLH, and MEOS enzyme activity in the rectum, colon, and small, and large intestine.
- Rectum had the highest ADH
- The small intestine had the lowest ADH
- Colon had some ADH
- The colon had the highest MEOS activity
- Rectum had MEOS activity
- Small intestines had the lowest MEOS activity
- Rectum small amounts of ALDH with high activity of ADH
- Large intestines accumulated acetaldehyde due to small amounts of ALDH
- Bacteria in the large intestines may activate ALDH and produce acetaldehyde
- Small Intestines had the highest activity with small amounts of ALDH
- Colon had less activity of ALDH
- Rectum had the most amount of ALDH but low activity
Alcohol metabolized without oxygen also occurs. This is less common and occurs when bacteria in the intestines interacts with fats.
Intestinal bacteria can produce large amounts of acetaldehyde from ADH. This occurs when alcohol is consumed in humans and rats.
Anaerobic bacteria will also produce acetaldehyde in the rectum.
How Alcohol Damages the Intestines
Acetaldehyde produces inflammation and damages the mucosa of the colon and rectum tissues. Cancer may also manifest in these areas as well.
ADH produced in the colon and rectum can also cause mucosal damage.
Alcohol Inflames and Changes The Intestines
Cell death caused by acetaldehyde leads to changes in the intestines that include the following:
- Sores on the intestine mucosa
- Intestinal erosions
- Loss of epithelium mainly at the villi tips
Inflammation from these conditions results in physical changes in the intestines:
- Alters the intestinal microbiome
- Increases intestinal permeability
- Disrupts intestinal mucosa immune system
Alcohol Alters the Intestinal Microbiome
Alcohol disrupts the bacterial balance. Dysbiosis and bacterial overgrowth in the intestines can occur.
Gram-negative bacteria produce lipopolysaccharides (LPS). These endotoxins will activate inflammatory proteins and cells.
Alcohol increases intestinal bacterial overgrowth in 2 ways:
- Directly by alcohol consumption
- Secondary to poor digestion and intestinal damage from alcohol consumption
Liver cirrhosis has abnormal intestinal motility and bacterial overgrowth.
Alcohol alters the bile-acid metabolism needed to regulate healthy bacteria.
Decreases in certain bile-acids were found in rats who consumed alcohol. Bacterial overgrowth was also reversed in rats with low bile acids.
Alcohol may alter the ratio of “good” to pathogenic bacteria.
Mice chronically fed alcohol had the following occur:
- Reductions in healthy bacteria
- Increases in endotoxin producing bacteria
Bacterial changes can induce intestinal alcohol metabolism and produce excess acetaldehyde in the colon. Furthermore, alcohol digestion byproducts increase the risk of intestinal inflammation.
Alcohol bloating is a result of bacterial overgrowth in the small intestine. Even moderate alcohol consumption. For example, having just 1 to 2 drinks can lead to changes in the gut.
Those with current alcohol consumption tested positive for small intestine bacterial overgrowth (SIBO) when compared with non-drinkers.
Consumption of healthy bacteria can prevent changes in the microbiome Alcohol-fed rats had shifts in bacteria balance when given Lactobacillus GG and probiotic oats.
Human and animal studies found pre and probiotics stimulate the growth of healthy bacteria and improve liver injury and dysfunction.
Alcohol Increases Intestinal Permeability
A protective barrier regulates what passes into the intestines. So it is somewhat permeable allowing for nutrient absorption. Consequently, intestinal permeability increases with the consumption of alcohol and a leaky gut can result.
Alcohol weakens the physical barrier of the intestine leading to gut leakiness. Therefore, mucus erosion from alcohol use could increase intestinal permeability.
Alcohol affects proteins that strengthen the mucosal barrier. It also increases the passage of endotoxins into the bloodstream.
Caco-2 are epithelial cells that indicate alcohol’s effect on intestinal permeability from alcohol consumption. When exposed to alcohol these cells show impairments of barrier function including:
- Increased oxidative stress
- Calcium release and MAP kinase activation
- Deplete zinc
- Activation of myosin light chain kinase (MLCK)
- MicroRNA 212 (miR-212) down-regulation of ZO-1
Acetaldehyde also contributed to leakiness in caco-2 cells.
Transepithelial and Paracellular Intestinal Damage From Alcohol
Alcohol and its byproducts damage cells of the intestinal barrier and increase intestinal permeability in the following ways:
- Transepithelial mechanisms – damage to epithelial cells
- Paracellular mechanisms – damage to tight junctions between cells
Direct cell damage is caused by transepithelial permeability. Cell membranes are weakened due to:
- Cell damage from DNA adducts formed from acetaldehyde
- Oxidative stress released from alcohol digestion
Paracellular permeability is caused by disruption to the tight junctions between intestinal barrier cells:
- Acetaldehyde weakens tight junctions by redistributing proteins
- Alcohol alters tight-junction proteins
- Aerobic alcohol metabolism redistributes tight junctions
Studies show alcohol weakens cytoskeletons the borders that give cells structure. This is because alcohol induces a leaky gut and disrupted tight junctional proteins in humans.
“Leaky gut” may be crucial to the development of chronic liver disease. Alcoholics with liver disease were the only ones with increased intestinal permeability.
Biopsies from cirrhotic livers showed large spaces below the tight junctions showing how long-term alcohol use affects intestinal permeability.
ZO-1 tight junction proteins decreases were associated with alcohol intake in rodents and alcoholics.
Alcohol Disrupts Circadian Rhythms and Increases Intestinal Permeability
Disruption of circadian rhythms in alcohol-fed mice worsened alcohol-related gut barrier dysfunction and increased intestinal dysbiosis, particularly when combined with another stressor such as a high-fat or high sugar diet.
Alcohol lowered total sleep time and increase sleep disruptions. Poor sleep patterns can affect melatonin levels. Melatonin regulates circadian rhythms.
Melatonin levels were low in those with alcohol intake. This correlated with increased permeability and endotoxin production.
Oats and Lactobacillus GG supplementation help maintain intestinal barrier strength. It prevents alcohol-induced stress on the intestinal cytoskeleton and tight junctions.
Alcohol Disrupts the Immune System in the Intestinal Mucosa
The intestinal barrier has an immunological function and will release antibodies as protection from toxins and pathogens. Alcoholics have increased levels of IgA antibodies. This response acts as a way to limit alcohol damage to the intestinal barrier.
Gut inflammation will result from this inflammatory response to alcohol and its metabolites leaving it susceptible to a host of pathogens.
Alcohol affects mucosal immunity in several ways:
- Decrease the innate and adaptive immune responses in the mucosa
- Cell cultures treated with alcohol produce inflammatory cells leukocytes and mast cells
- Endotoxins will bind to intestinal mucosa resulting in inflammation
- Modify gut immune responses both innate and adaptive
- Suppress immune defense cells
- Reduce antimicrobial secreting molecule
- Suppression of Interleukin-22 (needed for barrier function)
- Suppresses immune response and bacterial clearance
Alcohol inhibited the intestine’s immune response to removing hazardous bacteria in mice.
Modifications in immune responses further contribute to gut inflammation and the breakdown of the intestinal barrier.
Alcohol suppresses intestinal immune defense cells that secrete antibacterial compounds. Less of these compounds will lead to the growth of pathogenic bacteria and the production of endotoxins.
Intestinal permeability allows endotoxins to leave the gut and infiltrate other organs through the bloodstream.
Alcohol Inhibits Intestinal Enzyme Activity
Alcohol interferes with enzymes in the intestines:
- Lactase impairment causes a lactose deficiency
- Those enzymes that move nutrients into the bloodstream
- The enzyme that metabolizes drugs
- Enzymes that metabolize foreign substances
Other Effects of Alcohol on the Large Intestine
Alcohol consumption affects the colon’s muscle function in both animal and human studies. As a result, there can be reduced transit times which can cause diarrhea.
Dogs treated with alcohol had an increase in colon peristalsis while motility decreased. Muscle contractions significantly decreased in a section of the rectum in healthy humans given alcohol.
Effect of Alcohol on the Liver
After hitting the intestinal tract, alcohol moves to the liver through the portal vein.
The majority of alcohol digestion occurs in the liver. The liver is mainly responsible for eliminating alcohol from the body. There is little help from hormones.
The production of acetaldehyde and other toxic compounds increases inflammation and leads to liver damage.
Alcohol inflames the cells of the liver. After that swelling may occur. As a result there are blockages of the tiny passages to the small intestine prevent bile from getting to the liver.
Liver cells become destroyed with each drink of alcohol. Liver damage also lowers the rate of how fast alcohol can be digested and eliminated from the body.
Chronic alcohol consumption will lead to cirrhosis of the liver. Alcoholics are eight times more at risk for cirrhosis than non-alcoholics.
Endotoxins and proinflammatory cells can move to the liver when there is a leaky gut. Endotoxin levels in the liver increase following alcohol intake.
In response, liver cells will produce an immune response releasing their own cytokines. Inflammation will then ensue weakening the liver.

Alcohol Causes Nutrient Depletions & Deficiencies
Nutrient digestion and absorption can be disturbed due to alcohol consumption directly or as a consequence of increased intestinal permeability.
Vitamins may not be converted to their active form due to the toxic effects of alcohol on intestine and liver cells.
Alcohol vitamin depletion occurs in both chronic and moderate alcohol consumption. Additionally, alterations in protein, fat, and blood sugar are seen with the use of alcohol. The following nutrients are affected by alcohol intake:
- Vitamin A
- B complex vitamins
- Vitamin C
- Vitamin D
- Vitamin E
- Vitamin K
- Calcium
- Magnesium
- Iron
- Zinc
Alcohol Affects Protein, Blood Sugar, and Fat Status
Protein, blood sugar, and fat are impacted by alcohol intake.
Animal studies showed decreased absorption of water, sodium, glucose, fats, and some amino acids in the small intestine with limited alcohol exposure.
Cells need protein to function and grow. Alcohol weakens protein digestion and synthesis. Amino acid absorption impairment occurs in the small intestine and liver.
Glucose regulation is impaired with alcohol consumption. Fluctuations in blood sugar leading to hyperglycemia or hypoglycemia may occur. So continuous uncontrolled blood sugar can have negative consequences whether too low or too high.
Metabolites of alcohol digestion prevent glucose and amino acids from supplying energy to the brain and other body tissues when alcohol is consumed on an empty stomach.
Digestion and absorption of fats are also affected by alcohol consumption.
Alcohol Affects Vitamin Status
A poor intake of food occurs among heavy drinkers resulting in vitamin depletions. Metabolism and absorption of nutrients are also affected by damage to the digestive system from alcohol.
Pancreas and liver damage from the byproducts of alcohol metabolism can impair the digestion of nutrients.
Consequently, a decrease in nutrient absorption is due directly to alcohol intake. It can also be a result of impaired metabolism.
Alcohol Affects Water-Soluble Vitamin Status
In the small intestine, alcohol blocks the absorption of such substances as thiamin, folic acid, fat, vitamin B1, and vitamin B12.
So alcohol consumption may deplete all of the B complex vitamins:
- Thiamin (B1)
- Riboflavin (B3)
- Niacin (B3)
- Pantothenic acid (B5)
- Pyridoxine (B6)
- Biotin (B7)
- Folate (B9)
- Methylcobalamin (B12)
Chronic alcohol consumption resulted in unchanged or decreased thiamine, folate, and B12 status.
Folate deficiency can lead to anemia. GI damage can lead to poor absorption decreasing this nutrient.
Deficiency of B vitamins cause the following symptoms:
- B1 – Confusion, short-term memory loss, muscle weakness, enlarged heart
- B2- Skin disorders, swollen cracked lips, hair loss, sore throat,itchy and red eyes
- B3 – Pigmented rash, red tongue, apathy, headache, fatigue, loss of memory, depression
- B5 – Numbness and burning of extremities, headache, fatigue, irritability, poor sleep
- B6 – Poor immune function, cracks on the skin, fatigue, depression/anxiety
- B7 – Thinning hair, hair loss,red scaly rash around body openings, conjunctivitis;
- B9 – Fatigue, weakness, brain fog, irritability, headache, palpitations, shortness of breath
- B12 – Fatigue, dizziness, numbness in extremities, mood change
Alcohol Affects Fat-Soluble Vitamin Status
Fat-soluble vitamins require fat to be absorbed. Disruptions in fat metabolism vitamins A, D, E and K can become deficient.
Fat-soluble vitamin deficiencies cause the following complications:
- Night blindness
- Skin Rashes
- Poor Immunity
- Heavy bleeding and delayed blood clotting
- Neurological damage
- Weakened bones
- Wound healing
- Cell repair
Chronic alcohol consumption increases urinary losses of vitamin C leading to deficiency. Depletion of vitamin C is caused by chronic diarrhea or as subset of alcohol or chronic pancreatitis.
Alternatively, some small animal trials showed vitamin C may protect the liver from the effects of acetaldehyde. More trials need to be done to know if this would actually work.
Alcohol Affects Mineral Status
Deficiencies in the minerals calcium, magnesium, iron, and zinc often occur secondary to the effects of alcohol consumption.
Fat malabsorption decreases calcium levels.
Alcohol consumption acts as a diuretic for magnesium increasing urinary concentration of this nutrient. Therefore, chronic alcohol intake depletes body stores of magnesium.
Alcohol increases the iron transport and will accumulate in digestive organs. High iron levels inflame the esophagus and liver. Iron overload may produce oxidative damage and modify immune responses that can become carcinogenic.
Too much alcohol causes intestinal bleeding and results in iron deficiency.
ADH uses zinc to facilitate the production of acetaldehyde. This renders zinc powerless and unable to carry out any of its metabolic activities.
Depletions of zinc promoted carcinogenesis of the oro-esophageal in rats and mice. Low levels of zinc promotes carcinogenic pro-inflammatory genes and DNA in mouse and rat esophageal tissues.
Zinc supplementation can prevent oxidative stress that causes alcoholic liver injury.
Mineral deficiencies can lead to calcium-related bone disease, zinc-related night blindness, and skin lesions.

Alcohol and Hormones
Hormones control almost every cell and organ in the body. They are responsible to ensure homeostasis in body temperature, metabolism, energy production, growth, reproduction, stress management, and electrolyte balance.
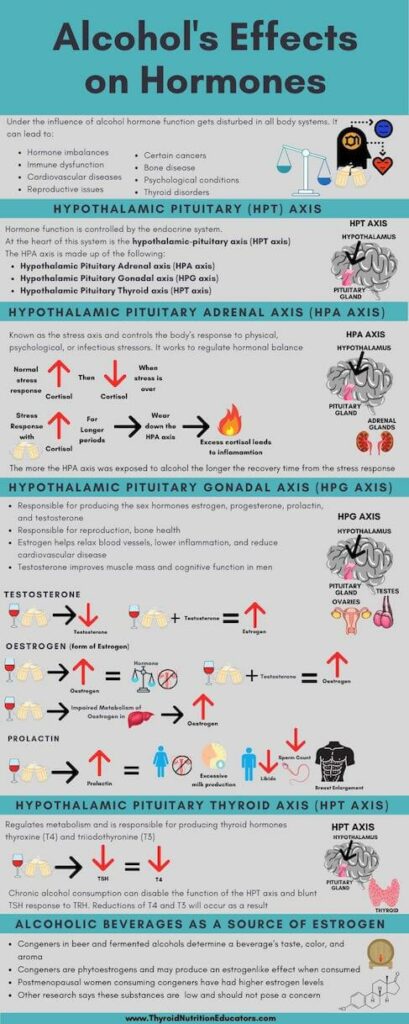
Under the influence of alcohol hormone function gets disturbed in all body systems. It can lead to hormone imbalances, immune dysfunction, cardiovascular diseases, reproductive issues, certain cancers, bone disease, psychological conditions, and of course thyroid disorders.
Hypothalamic Pituitary Axis (HPT Axis)
Hormone function is controlled by the endocrine system. At the heart of this system is the hypothalamic-pituitary axis (HPT axis) the which is made up of the following:
- (HPA axis) Hypothalamic Pituitary Adrenal axis
- (HPG axis) Hypothalamic Pituitary Gonadal axis
- (HPT axis) Hypothalamic Pituitary Thyroid axis
(HPA Axis) Hypothalamic Pituitary Adrenal Axis and Alcohol Consumption
The Hypothalamic Pituitary Adrenal axis (HPA axis) is known as the stress axis and controls the body’s response to physical, psychological, or infectious stressors. It works to regulate hormonal balance:
- Hypothalamus secretes corticotropin-releasing hormone (CRH)
- Adrenocorticotropic hormone (ACTH) is secreted from cells in the pituitary gland
- ACTH moves to the adrenals glands and triggers the production of cortisol
- Cortisol triggers a negative feedback loop
- Cortisol receptor activity will increase in the pituitary, hypothalamus, and hippocampus
- The nervous system produces β-endorphin (BEP) in the hypothalamus
- BEP binds to pituitary opioid receptors and HPA activity will be hindered
- The hippocampus and pituitary decrease CRH and ACTH shutting off the stress response
A normal stress response is accompanied by a quick rise in cortisol levels and a rapid decline when the stressful event is over.
HPA Axis Is Worn Down By The Stress Response
Overproduction of the stress response can not only wear down the effects of the HPA axis but expose the body to excess cortisol and pro-inflammatory substances.
Alcohol use can also wear down the HPA axis:
- Alcohol can elevate cortisol in healthy subjects at doses over 100 mg
- Men with self-reported alcohol consumption had higher urinary levels of cortisol
- HPA Axis is impaired in heavy drinkers
Similarly, the HPA axis in rats was altered by several weeks of 30 minutes of self-administered drinking:
- Cortisol was elevated within 15 minutes of consumption
- As blood alcohol level increases, high cortisol levels will also develop
- HPA hormone levels were eventually elevated
- Low and Moderate drinking affected HPA function somewhat
- Chronic exposure resulted in significant impairment of HPA function
The more the HPA axis was exposed to alcohol the longer the recovery time from the stress response.
Hypothalamic Pituitary Gonadal axis (HPG axis) and Alcohol
The hypothalamic-pituitary-gonadal axis (HPG axis) is responsible for producing gonadotropin-releasing hormone (GnRH) or luteinizing hormone-releasing hormone (LHRH).
LHRH is secreted into the pituitary gland and binds to receptors on gonadotroph cells.
LHRH produces two important hormones follicle-stimulating hormone (FSH) and luteinizing hormone (LH).
FSH and LH create sex hormones estrogen, progesterone, prolactin, and testosterone. Their production is controlled by a feedback loop and will act on the hypothalamus and pituitary to either inhibit or stimulate the release of LHRH, LH, and FSH.
Aside from reproduction, these hormones also play important roles in other physiological processes.
Estrogen, progesterone, and testosterone are needed to maintain bone health. Estrogen helps relax blood vessels, lower inflammation, and reduce cardiovascular disease. Testosterone helps improve muscle mass and cognitive function in adult men.
Alcohol affects the HPG axis leading to a dysfunction in both men and women.
Oestrogen (Estrogen) and Alcohol Intake
Alcohol intake increases the levels of oestrogen in the body. Oestrogen is a form of estrogen.
Alcohol intake increases oestrogen levels and can affect the pre- and postmenopausal women.
Oestrogen is produced by the ovaries and has been shown to be disturbed with alcohol consumption.
Alcohol increases oestrogen levels in two possible ways:
- Increasing enzymes that turn androgens into the oestrogens
- Impairing the metabolism of oestrogen in the liver
Oestrogen Level Increased by Alcohol Intake
Alcohol puts a strain on the liver limiting its ability to clear the increased production of oestrogens from the body. Therefore, oestrogen builds up in body cells and creates hormone imbalances in both men and women.
Moderate alcohol use puts premenopausal women at risk for missed and/or irregular menstrual cycles, risk of miscarriage, and early menopause.
Five or fewer drinks a week decreased pregnancy in healthy women 20 to 35 years old.
Significant disturbances in hormones and menstrual cycles were seen in social and heavy drinking healthy nonalcoholic women when compared with occasional drinkers (less than 3 drinks per day)
- 50% of social drinkers (~3.84 drinks per day) had no cycle
- 60% of heavy drinkers (~7.81 drinks per day) had elevated prolactin levels
Long-term moderate intake of alcohol decreased ovarian reserves and increased FSH levels. The hormone responsible for estrogen production
Acetaldehyde produced from alcohol metabolism may damage ovaries. Rats given alcohol were found to have aldehyde dehydrogenase activity and oxidative cell damage.
Alcohol intake temporarily increases estrogen in postmenopausal women receiving hormone therapy possibly due to impaired estrogen metabolism. No effect was seen in those not receiving hormone therapy.
So if your client is suffering from already high levels of estrogen and oestrogen alcohol intake could elevate their levels making it worse.
Testosterone and Alcohol Intake
Alcohol lowers testosterone levels in men.
Chronic alcohol consumption in young male rats had cell damage in the pituitary gland affecting testosterone production.
Acetaldehyde produced from alcohol digestion was found to stop the production of enzymes needed for testosterone production.
Chronic alcohol consumption significantly decreased testosterone in both alcoholic and non-alcoholic men.
Alcohol increases the conversion of testosterone to estrogens, especially in the liver. Elevated estrogens can increase the incidence of feminization in men.
Prolactin and Alcohol Intake
Alcohol was also found to affect prolactin levels in both men and women. Levels should be minimal in healthy individuals. Elevated levels lead to hormone dysfunction:
- Women: amenorrhea, excessive milk production
- Men: decreased sex drive, low sperm count, impotence, and breast enlargement
Hypothalamic Pituitary Thyroid Axis (HPT axis) and Alcohol
The hypothalamic-pituitary-thyroid axis (HPT axis) regulates metabolism in every cell in the body. It is responsible for producing thyroid hormones thyroxine (T4) and triiodothyronine (T3).
When T4 and T3 are low the hypothalamus will release thyrotropin-releasing hormone (TRH). TRH will tell the cells of the anterior pituitary to produce and secrete thyroid-stimulating hormone (TSH). TSH will tell the thyroid to produce and secrete T4 and T3.
Thyroid hormones T4 and T3 levels are regulated by a negative feedback loop at the hypothalamus and pituitary:
- Low thyroid hormone levels, TSH will START hormone production and secretion
- High thyroid hormone levels,TSH will STOP hormone production and secretion
Chronic alcohol consumption can disable the function of the HPT axis and blunt TSH response to TRH. Reductions of T4 and T3 will occur as a result.
Alcoholic Beverages As a Source of Estrogen
There has been speculation that there may be estrogen in beer and other fermented alcohols. These congeners are substances that determine a beverage’s taste, color, and aroma. Some congeners are phytoestrogens and produce an estrogen-like effect when consumed.
Heavy drinking has been associated with feminization in men due to alcohol’s estrogenic effect.
The estrogenic effects of congeners in bourbon and red wine may also produce estrogenic effects in moderate drinkers.
Twenty-four postmenopausal estrogen-deficient women aged 57 to 59 years old were found to have higher hormone levels of estrogen after consuming one drink of white wine congeners, red wine congeners, beer congeners, or bourbon congeners nightly for 4 weeks.
Effects of each congener did not differ and hormone levels stabilized one week after the last day the congener was consumed.
Other research says the levels of phytoestrogens in beer are low and should not pose a concern.
Alcohol and the Immune System
Any alcohol intake has been shown to suppress the immune system. Alcohol elevates cortisol. High levels of cortisol compromise immune function and alter cell metabolism.
Two ways alcohol induces inflammation include:
- LPS produced from toxic bacteria in the gut increase inflammation
- Oxidation and cell damage from alcohol metabolism trigger the production of pro-inflammatory cytokines (TNF-α and IL-6)
Most immune dysfunction that occurs due to alcohol intake is a result of a weakened HPA axis to external stressors such as infections.
HPA Axis and The Immune System
The HPA axis is also responsible for a healthy functioning immune system.
CRH and ACTH have immuno-protective benefits that calm inflammatory processes.
Immune fighting cells activate the HPA axis and CRH and ACTH secretion through a feedback loop. The immune system relies on the HPA axis for an adequate immune response.
Constant cortisol production from alcohol consumption weakens the HPA axis interferes with immune system cell signaling.
Alcohol abuse hinders both of these systems. Long-term alcohol use is associated with alterations in the HPA axis and immune system function.
Low/Moderate Alcohol Intake & Immune Function
Alcohol reduces the number of white blood cells and their ability to fight infection.
Short-term exposure leads to suppression of certain cytokines including TNF-α and IL 1ß.
Chronic Alcohol Use and Immune Function
Alcohol abuse disorders are associated with chronic systemic inflammation, elevated pro-inflammatory immune cells, and cortisol production are associated.
Chronic intake lowers white blood cell activity despite the increase in the number of cells. Other immune-fighting cells are also decreased and weakened.
Long-term exposure is associated with the production of the pro-inflammatory cytokines TNF-α. It suppresses the production of proteins that attract white blood cell production such as chemokines.

Now we know there are a lot of effects of alcohol on the digestive system. Now we will discuss how alcohol affects the thyroid.
Alcohol and the Thyroid
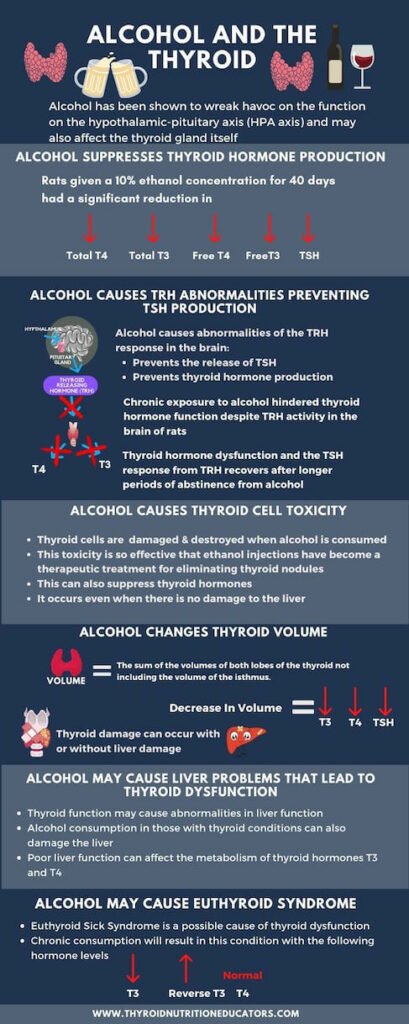
Alcohol has been shown to wreak havoc on the function on the hypothalamic-pituitary axis (HPA axis) so may also affect the thyroid gland itself.
Drinking alcohol affects the thyroid gland in the following ways:
- Suppresses or blocks thyroid hormone production
- Cause TRH abnormalities that block TSH production
- Thyroid cell toxicity
- Changes in thyroid volume
- Causes Euthyroid Syndrome
- Liver conditions may increase thyroid dysfunction
Alcohol Suppresses Thyroid Hormone Production
Both T4 and T3 become suppressed with chronic alcohol intake. T4 to a lesser extent than T3.
Moderate drinking also showed a depression in T4 levels.
Rats given a 10% ethanol concentration for 40 days had a significant reduction in total T4, total T3, free T4, T3, and TSH when compared to controls.
Alcohol abuse will also affect thyroid hormone levels.
Reductions in free T3 and T4 result from heavy alcohol consumption and maybe a marker of chronic alcoholism in those with a family history.
Withdrawal from alcohol showed a significant reduction in T4 and T3 when compared with nonalcoholic healthy individuals.
Alcohol Causes Prevents TSH Production
Alcohol causes abnormalities of the TRH response preventing the release of TSH and thyroid hormones. Thyroid dysfunction will occur as a result of this.
TRH stimulates TSH and thyroid hormone production. When inhibited the thyroid gland will not produce any hormone.
Chronic exposure to alcohol hindered thyroid hormone function despite TRH activity in the brain of rats.
Alcohol may also reduce receptor activity preventing the TSH response to TRH.
Thyroid hormone dysfunction and the TSH response from TRH recovers after longer periods of abstinence from alcohol.
Rats given alcohol for 40 days had a significant decrease in TSH, total T4, total T3, free T4, and free T3 when compared to control animals.
Thyroid Cell Toxicity From Alcohol Consumption
Alcohol damages and destroys thyroid cells. This toxicity is so effective that ethanol injections have become a therapeutic treatment for eliminating thyroid nodules.
Thyroid cell toxicity can also suppress thyroid hormones. It occurs even when there is no damage to the liver.
Toxicity from alcohol may also lead to a reduction in thyroid volume.
Alcohol Changes the Thyroid Volume
The thyroid volume is the sum of the volumes of both lobes of the thyroid not including the volume of the isthmus.
The thyroid volume is determined with a thyroid ultrasound.
T3, Free T3, and thyroid gland volume significantly decreased in alcoholics with cirrhosis of the liver when compared with normal subjects [R].
TSH levels increased in those with liver cirrhosis when compared with healthy individuals.
Thyroid volume also decreases due to alcohol-induced thyroid fibrosis. Chronic alcohol users have more fibrosis than occasional binge drinkers. So the dose makes the poison when it comes to thyroid fibrosis.
Reductions in size are accompanied by decreases in T3 and free T3 hormones. T4, free T4, and TSH.
Thyroid fibrosis can occur without liver cirrhosis or other damage. Those with non-alcoholic liver cirrhosis do not have changes in thyroid volume when compared to controls.
So thyroid damage can occur with or without liver damage.
Alcohol, Liver Problems, & Thyroid Dysfunction
Thyroid function may cause abnormalities in liver function. Alcohol consumption in those with thyroid conditions can also damage the liver. Poor liver function can affect the metabolism of thyroid hormones T3 and T4.
Alcohol May Cause Euthyroid Syndrome
Another possible cause of alcohol-induced thyroid dysfunction is due to Euthyroid Sick Syndrome.
Chronic consumption will result in Euthyroid Sick Syndrome. Signs normal T4, suppressed T3, and high levels of reverse T3 (rT3).
Alcohol’s Effect on Thyroid Diseases
Knowing the effects of alcohol on the thyroid, those with existing thyroid and other hormonal dysfunction could be at risk when consuming alcohol.
Alcohol and Hypothyroidism/Hyperthyroidism
Research on thyroid disease is limited. Mostly, it deals more with the effects of alcohol on the HPT axis and how it suppresses thyroid hormone function and inhibits thyroid hormone metabolism in the liver.
Alcohol has been correlated with lower incidences of hypo-, hyperthyroidism, and autoimmune thyroid diseases in observational studies. This does not mean alcohol is the cause for preventing thyroid dysfunction.
Additionally, excess alcohol consumption is damaging to those with any thyroid condition.
Long-term alcohol intake can hamper thyroid function lowering TSH and T4 levels. As consumption increases thyroid function wanes creating less hormone [R].
Alcohol consumption may put those with already low TSH and/or T4 levels at risk.
Alcohol and Autoimmune Thyroid Diseases
The association of alcohol and autoimmune thyroid diseases has not been studied in depth Observational research shows a protective effect with moderate consumption.
Alcohol in doses of up to 3 drinks of beer and/or wine per day may possibly prevent autoimmune hypothyroidism in both men and women 60 years and younger [R].
Higher consumption did not protect against thyroid conditions and may be harmful to health. High intake of alcohol was associated with positive antibodies in women.
There is more information on alcohol and hyperthyroidism and how alcohol affects Graves’ disease.
The relationship between Graves’ disease and alcohol shows both positive and negative outcomes.
Moderate alcohol consumption may also have a protective effect against Graves’ hyperthyroidism.
Lower incidences of Graves’ hyperthyroidism were in those who consumed less than 6 drinks per week.
Those with Graves’ disease also reported alcohol consumption once or more during the week.
A few studies also found no association between moderate drinking and Graves’ disease prevention.
Food frequency questionnaires of 543 women with Graves’ hyperthyroidism in the Nurses’ Health Study found no benefit from alcohol on the thyroid. Another observational study of 301 individuals with Graves’ showed no association with alcohol consumption.

Health Conditions Secondary to Alcohol’s Thyroid Damage
Secondary health conditions can result from alcohol damage making a bad thyroid worse. These include weight gain, elevated blood sugar, heart palpitations, and cognitive and mood functions.
Thyroid and Weight Gain Secondary to Alcohol
Thyroid and weight gain is a combination seen with increases in the intake of alcohol. This is because alcohol affects metabolism.
Dysfunction of the thyroid and weight gain go hand in hand. The addition of alcohol may further weaken the thyroid resulting in changes in weight, composition, body temperature, and total and resting energy expenditure (REE).
Weight gain from alcohol can affect thyroid function and increase the risk of thyroid disorders. Obesity may be a risk for hypothyroidism and thyroid autoimmune conditions.
Thyroid and Heart Palpitations Secondary to Alcohol
Excess alcohol consumption can affect the health of the heart. Thyroid dysfunction affects the cardiovascular system.
Hypothyroidism can lower cardiac output, slow heart rate, increase blood pressure, promote atherosclerosis, impair muscle function, and decrease stroke volume.
There is a connection between alcohol, thyroid, and heart palpitations in conditions like hyperthyroidism and Graves’ disease.
Excess thyroid hormone in hyperthyroid conditions like Graves causes the heart to beat faster. This may lead to abnormal rhythms including atrial fibrillation.
Thyroid and Blood Sugar Changes Secondary to Alcohol’s Damage
Thyroid, and blood sugar levels are affected by alcohol consumption.
Metabolic dysfunction occurs in both thyroid conditions and alcohol consumption. Impaired thyroid hormone function may result in changes in blood sugar. Those with diabetes may also have changes in their HbA1C. Those with thyroid conditions who consume alcohol may have an increased risk for metabolic syndrome and changes in blood sugar levels.
Thyroid and Sleep Disorders Secondary to Alcohol’s Damage
TSH and thyroid hormone production are controlled by circadian rhythms. Any dysfunction in the thyroid will also affect sleep.
Alcohol disrupts sleep by impairing circadian rhythms, lowering total sleep, and increasing disruptions.
The combination of thyroid disorders and alcohol consumption may lead to poor sleep and disruption of TSH secretion.
Sleep in rats with hypothyroidism was found to decrease by 16% when given alcohol.
Clients with sleeping issues and thyroid problems may want to evaluate their alcohol intake.
Thyroid and Mood Disorders Secondary to Alcohol’s Damage
Changes in mood occur in those with thyroid conditions. Alcohol alters brain chemistry resulting in depression and other mood disorders.
It is unclear whether alcohol abuse causes depression or depression leads to alcohol abuse. Alcohol’s depressant effects can affect the thyroid when consumed in excess.
Clients with clients suffering from depression may benefit from a thyroid screening and alcohol intake evaluation.

Alcohol Effects on a Thyroid Blood Test
Alcohol’s effects on thyroid hormones may alter a thyroid blood test.
Serum TSH and T4 decrease after chronic alcohol consumption. These reductions in thyroid hormone may result from damage to the HPTA axis or the thyroid gland itself.
Alcohol and Thyroid Medication
Like other medications, interactions between alcohol and thyroid medication may occur.
Hypothyroid Medications
There are various hypothyroid medications. Here we will discuss the connection between alcohol and thyroid medications.
- Levothyroxine and Alcohol: no specific interactions
- Synthroid and Alcohol no specific interactions between
- Armour Thyroid and Alcohol: no specific interactions
- Desiccated Thyroid (NP Thyroid) and Alcohol: no specific interactions
Though alcohol does not interact with thyroid medications may affect liver health.
In very rare cases Levothyroxine was found to cause liver injury. Liver function returned to normal after stopping this medication.
Abnormal liver function tests were rare in the use of Armour thyroid.
NP thyroid, Armour, Synthroid, and levothyroxine interactions may occur in the presence of certain health conditions including diabetes, adrenal gland insufficiency, heart disease, anemia, blood clotting problems, osteoporosis, heart arrhythmias, atrial fibrillation, and adrenal and pituitary problems.
Hyperthyroid Medications
Hyperthyroid medications are given to those with an overactive thyroid. They include Methimazole and Carbimazole.
Methimazole and Alcohol
There are no specific side effects from the combination of Methimazole and alcohol.
Methimazole is less likely to affect liver enzymes but may lead to cholestasis. This reduction in bile from liver cells to the small intestine will build up in the liver and impair its function.
Carbimazole and Alcohol
There are no specific side effects from the combination Carbimazole and alcohol.
Bilirubin, alkaline phosphatase, and γ‐glutamyl transpeptidase levels may become elevated within 2 to 3 weeks of starting treatment and can last for several months even after discontinuation.
The liver metabolizes medications. Clients on multiple medications should have liver status checked routinely to check for any abnormalities. Limit alcohol in those with thyroid conditions. Check the function of the thyroid and liver within three months of treatment.

How Gluten in Alcohol May Affect Thyroid Function
Gliadin and gluten found in alcohol may be more damaging to the thyroid than other alcoholic beverages.
Gluten and gliadin are found in wheat, oats, barley, and rye. These compounds are also in certain beers, wines, and liquors.
Those with thyroid conditions can have an intolerance to gluten and gliadin. Effects of gluten and gliadin digestion are similar to that of alcohol metabolism.
Effects of Gluten In Alcohol on Thyroid Health
Consumption of gliadin and gluten weakens the health of the gut. When consumed these proteins produce a substance called zonulin which is responsible for opening the tight junctions.
The more zonulin produced, the longer the intestinal barrier is open resulting in a leaky gut.
If someone has a drink with gluten there will be an inflammatory effect not only from alcohol but also from the gluten and gliadin particles further perpetuating a thyroid condition.
It is not the quantity but the presence of these proteins that cause damage. So any amount can produce zonulin. Zonulin increases inflammation.
Eliminating gluten improved thyroid dysfunction in 71% of those with leaky gut.
Types of Gluten-Free Alcohol
When choosing alcoholic beverages look for gluten-free alcohol instead.
There are many options for versions of gluten-free alcohol.
Gluten-free Beer
Beer is fermented with barley and hops that contain gluten.
Malted beverages and wine coolers also contain gluten.
Some malted beverages that contain barley may say “gluten-removed” during processing. These will still contain traces of gluten and may be problematic for those with gluten intolerances.
Ciders are beers that are naturally gluten-free.
Wine is Naturally Gluten-Free
Wine is naturally gluten-free. It does not contain any gluten.
Fermentation does not use any gluten. Wheatpaste may be used to seal oak barrels. The amount is much less than the FDA-mandated gluten-free requirements (<20 parts per million) and does not touch the wine.
Fining and clarifying wine techniques that may use gluten. Most gluten will be removed from the wine. Any remaining particles are too small to be considered gluten-free. Studies show levels are too low to cause problems.
However, it is best to ask your clients if any specific alcohol may be affecting them.
Rice wine known as “sake” is gluten-free. It is made from fermented rice.
Some wine drinks are NOT gluten-free. Wine coolers, “flavored” wine beverages, and wine cocktails may contain gluten.
Gluten-Free Liquor and Mixers
Gluten-free liquor includes anything that is made from gluten-free foods.
Distilled liquors even those made from wheat, barley, or rye are also gluten-free. The distillation process removes gluten. Those with wheat sensitivities may still want to avoid certain beverages.
Gluten-free liquors (after distillation) include the following:
- Bourbon (some brands still contain wheat)
- Whiskey/Whisky (some brands still contain wheat)
- Tequila (100% agave naturally gluten free
- Gin (some brands still contain wheat)
- Vodka (potato, rice, fig are naturally gluten free
- Rum (some brands still contain wheat)
- Cognac (some brands still contain wheat)
- Brandy (some brands still contain wheat)
- Absinthe (some brands still contain wheat)
- Mezcal (some brands still contain wheat)
- Scotch (some brands still contain wheat)
- Vermouth (some brands still contain wheat)
- Liqueur (some brands still contain wheat)
Gluten may STILL be lurking in liquors with gluten-containing ingredients added AFTER the distillation process. Added flavors or other additives after distillation may have gluten-containing ingredients.
Cross-contamination may also occur in facilities that process products containing wheat, barley, or rye.

Possible Benefits of Alcohol for the Thyroid
Alcohol has shown some protective benefit in the prevention of goiter and thyroid nodules.
On the other hand, there are also many studies that show alcohol may protect from thyroid cancer as well.
This does not discredit all the negative effects alcohol has on the body and thyroid health.
Long-term heavy drinking is toxic and may cause cancer. A 30-year study found those who drank were more likely to get thyroid cancer than non-drinkers.
Alcohol consumption may prevent autoimmune thyroid diseases.
Moderate consumption was seen to protect against autoimmune thyroid diseases such as Hashimoto’s and Graves’ disease as seen above.
Excess consumption in greater amounts than 3 to 6 drinks per day also has a negative effect on the immune system and results in systemic inflammation.
Alcohol Recommendations
Light drinking may have shown protective benefits. Others feel that alcohol can be a risk for many health conditions and has no therapeutic value.
When it comes to alcohol recommendations it varies depending on the client.
Knowing how much alcohol your client consumes is key to understanding how it may affect thyroid function.
Alcohol Recommendations Should be Individualized
Like nutrition, alcohol recommendations should be individualized and vary depending on a person’s health.
Alcohol Recommendations for Healthy Individuals
Healthy individuals should follow the following moderate drinking recommendations:
- Men: 2 drinks per day
- Women: 1 drink per day
What is A Standard Drink
A standard drink is any drink that contains about 0.6 fluid ounces or 14 grams of pure alcohol. The following are standard drinks:
- 12 ounces of regular beer (about 5% alcohol)
- 8-9 ounces of malt liquor (about 7% alcohol)
- 5 ounces of wine (about 12% alcohol)
- 3-4 fl oz of fortified wine, such as sherry or port (about 17% alcohol)
- 2-3 fl oz of cordial, liqueur, or aperitif (about 24% alcohol)
- 1.5 fl oz of brandy or cognac (about 24% alcohol)
- 1.5 ounces 80-proof distilled liquor (up to 40% alcohol)

How Much is Too Much Alcohol
The problem with alcohol is we often lose track of how much we are consuming. Like regular beverages, multiple servings of alcohol can be found within just one container.
To know how much your client is consuming here is a list of a number of beverages found in various containers:
Number of Drinks in Beer
- 12 fl oz = 1 drink
- 16 fl oz = 1 ⅓
- 22 fl oz = 2
- 40 fl oz = 3 ⅓
Number of Drinks in Malt Liquor
- 12 fl oz = 1 ½
- 16 fl oz = 2
- 22 fl oz = 2 ½
- 40 fl oz = 4 ½
Number of Drinks in Wine
- 750 ml (a regular wine bottle) = 5 drinks
Number of Drinks in Liquor
- 1.5 oz shot per 50-ml bottle = 1
- A mixed drink or cocktail = 1 or more
- 200 ml (a “half pint”) = 4 ½
- 375 ml (a “pint” or “half bottle”) = 8 ½
- 750 ml (a “fifth”) = 17
What Constitutes Binge and Excessive Drinking?
Binge drinking and heavy alcohol use can be dangerous even for healthy individuals.
Binge drinking consists of having a blood alcohol concentration (BAC) to 0.08% or higher it typically occurs after the following consumption within 2 hours:
- Women: 4 drinks
- Men 5 drinks
Heavy alcohol is drinking the following on any given day:
- Women: more than 3 drinks
- Men: more than 4 drinks
Excessive drinking consists of binge drinking and heavy alcohol use. It increases the risk of health conditions and alcohol dependence. As alcohol intake increases so does the risk.
Women More At Risk For Negative Affects of Alcohol Than Men
A higher percentage of women tend to have thyroid conditions. Women are also more susceptible to the perils of alcohol’s effects.
This is very frustrating but something to look out for in your clients when assessing alcohol intake.
Not to say that men do not have to worry. More and more men are getting thyroid conditions and also need to be aware of the risks of alcohol intake.
One suggestion is not to use alcohol as stress relief.
Don’t Use Alcohol for Stress Relief and as Self-Care
Wine is often marketed as a form of self-care. One glass can turn into 2 and the next thing you know the whole bottle is gone.
Don’t let it become a tool for stress relief. Look at your client’s intake and see if this is something that is being used to reduce their stress levels. If so, it could be hurting their thyroid health.

Alcohol Recommendations for Those with Thyroid Conditions
Alcohol metabolism has negative effects on healthy individuals. Especially if someone is consuming alcohol at high levels on a daily basis.
So it can be hard to recommend daily consumption for anyone on medications and with compromised health. They may not be able to physically handle its toxic effects.
If your clients already are nondrinkers there is no reason for them to start drinking. For those that drink it is best to evaluate any thyroid-like symptoms, they may have.
Some with thyroid conditions need to take caution and possibly avoid alcohol consumption especially if they have not started taking care of their nutrition yet.
If someone is suffering from leaky gut, elevated liver enzymes, elevated antibodies, and suppressed thyroid hormone function it is not recommended to have any alcohol.
Those who are further along on their journey and have started to heal their gut may do fine with an occasional drink.
It is important to give them the facts. Tell them how alcohol affects gut and thyroid health and consumption can hinder health improvements.
If your client is not able to abstain from alcohol the best thing to do is stick to minimal intake and see how it affects them by having them listen to their body.
Listen to the Body When It Comes to Alcohol Intake
Have your clients listen to their bodies after consumption to see how alcohol affects them.
Do they feel fatigued, low energy, or had a bad hangover after just one drink? If so, the alcohol has to go.
If they are exhibiting signs of thyroid dysfunction look at their alcohol intake and scale back to make improvements.
Autoimmune Thyroid Disease Alcohol Recommendations
Since alcohol affects the immune system, those with a history of both autoimmune and thyroid conditions should go easy on the alcohol consumption for risk of chronic inflammatory conditions involving the thyroid.
If you are in a state of inflammation and are producing antibodies drinking may not be the best thing to do.
Anecdotal evidence of negative alcohol intolerance has been found in those with all thyroid conditions. Intake may result in alcohol sensitivity or intolerance for some individuals.
No Thyroid Condition But Symptomatic Alcohol Recommendations
If a client is not diagnosed with a thyroid condition but is exhibiting symptoms of a thyroid condition you If someone exhibits symptoms of a thyroid condition but is not diagnosed.
Thyroid Experts Alcohol Recommendations
Thyroid experts agree those with thyroid conditions should limit or abstain from daily alcohol intake until thyroid health has improved.
Isabella Wentz, The Thyroid Pharmacist, and Hashimoto’s expert feel that alcohol contributes to a leaky gut, blood sugar imbalances, SIBO, and backlog in the liver. Drinking even small amounts of alcohol may make someone with a thyroid condition feel awful the next day.
Amy Myers, MD, a functional medicine physician feels that alcohol is toxic that should be cleansed of the system. It suppresses the central nervous system and leads to a weakened immune system, leaky gut, and interferes with causing malabsorption. Recommendations are for only 1 to 2 drinks per week.

The Effect of Diet on Alcohol and the Thyroid
A poor diet counteracts any benefit of alcohol. That is because certain foods like gluten, dairy, and polyunsaturated oils may promote inflammation already set off by alcohol metabolism.
Summary
Alcohol has been shown to have negative effects on multiple body systems leading to:
- Altered metabolism of proteins, fats, and carbohydrates
- Decreased absorption of nutrients essential to the thyroid
- Higher levels of pathogenic bacteria
- An increase in inflammatory responses
- Increase in incidence of leaky gut
- Suppressed thyroid function
- Weakend HPA, HPT, and HPG axis
- Hormonal imbalances
The byproducts of alcohol metabolism are toxic so moderate drinking is recommended for healthy individuals. However, those with thyroid conditions may need to limit their intake depending on symptoms.
In addition, moderate alcohol consumption may also inhibit certain autoimmune thyroid disorders. There is no evidence as to why this occurs.
Those on medications and with thyroid dysfunction may be more susceptible to the damage of alcohol and should abstain or limit their alcohol intake depending on the health of their thyroid
More Thyroid Nutrition Articles
- Functional Nutrition for Thyroid
- Best Foods for Thyroid Patients
- Should Your Clients go Gluten Free
- Mushroom Supplements for Thyroid Nutrition
- Infrared Sauna Benefits
- Mock Meat and the Thyroid
- What Are Optimal Thyroid Levels
- Signs of a Thyroid Condition
- Probiotics for Thyroid Health
- Thyroid and Eczema
The information on this website has not been evaluated by the Food & Drug Administration or any other medical body. It is shared for educational purposes only and is not intended to diagnose, treat, prevent, or cure any disease. Consult your doctor or healthcare provider before making changes to your diet, exercise regimen or lifestyle. By accessing or using this website, you agree to abide by the Terms of Service, Full Disclaimer, and Privacy Policy. Content may not be reproduced in any form.

